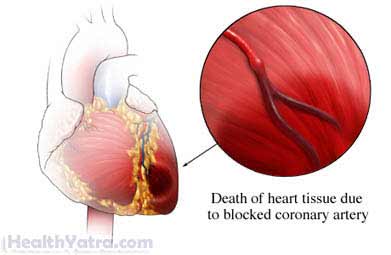
Definition
A heart attack occurs when blood flow to the heart muscle is interrupted. Oxygen cannot get to the heart muscle, causing tissue damage or tissue death.
Causes
A heart attack may be caused by:
- Thickening of the walls of the arteries feeding the heart muscle (coronary arteries)
- Accumulation of fatty plaques in the coronary arteries
- Narrowing of the coronary arteries
- Spasm of the coronary arteries
- Development of a blood clot in the coronary arteries
- Embolism that affects the coronary arteries
Risk Factors
These factors increase your chance of developing heart attack. Tell your doctor if you have any of these:
- Sex: male
- Increased age
- Obesity
- Smoking
- High blood pressure
- Sedentary lifestyle
- High blood cholesterol (specifically, high LDL cholesterol, and low HDL cholesterol)
- High blood triglycerides
- Diabetes
- Stress
- Family members with heart disease
Symptoms
Symptoms include:
- Squeezing, heavy chest pain, especially with:
- Exercise or exertion
- Emotional stress
- Cold weather
- A large meal
- Pain in the left shoulder, left arm, or jaw
- Shortness of breath
- Sweating, clammy skin
- Nausea
- Weakness
- Loss of consciousness
- Anxiety, especially feeling a sense of doom or panic without apparent reason
Unusual symptoms of heart attack (may occur more frequently in women):
- Stomach pain
- Back and shoulder pain
- Confusion
- Fainting
If you think you are having a heart attack, call 911 right away.
Diagnosis
Tests may include:
- Blood tests—To look for certain enzymes found in the blood within hours or days after a heart attack.
- Urine tests—To look for certain substances found in the urine within hours or days after a heart attack.
- Electrocardiogram (EKG)—Records the heart’s activity by measuring electrical currents through the heart muscle, changes can show if there is blockage or damage.
- Echocardiogram—Uses high-frequency sound waves (ultrasound) to examine the size, shape, function, and motion of the heart.
- Stress test—Records the heart’s electrical activity under increased physical stress, usually done days or weeks after the heart attack.
- Nuclear scanning—Uses radioactive material to show areas of the heart muscle where there is diminished blood flow.
- Electron-beam computed tomography (EBCT)—A type of x-ray that uses a computer to make detailed pictures of the heart, coronary arteries, and surrounding structures.
- Coronary angiography—Uses dye and x-rays to look for narrowing or blockage in the coronary arteries.
Treatment
Treatment includes:
- Oxygen
- Pain-relieving medicine
- Nitrate medicines
- Aspirin and other antiplatelet agents
- Beta-blockers and/or angiotensin-converting enzyme (ACE) inhibitor medicines
- Anti-anxiety medicine
- Cholesterol-lowering medicines (such as statin drugs)
Within the first six hours after a heart attack, you may be given medicines to break up blood clots in the coronary arteries. Other medicines that may be given include those that block the function of platelets.
Surgery
If you have severe blockages, you may need surgery, such as:
- Coronary artery bypass grafting (CABG)
- Atherectomy
- Balloon angioplasty with or without stenting
Physical or Rehabilitative Therapy
During recovery, you may need physical or rehabilitative therapy to help you regain your strength.
Treatment for Depression
You may feel depressed after having a heart attack. Therapy and medicine can help relieve depression.
If you have a heart attack, follow your doctor’s instructions .
Prevention
Preventing or treating coronary artery disease may help prevent a heart attack.
- Maintain a healthy weight.
- Begin a safe exercise program. Follow your doctor’s advice.
- If you smoke, quit.
- Eat a healthy diet. Your diet should be low in saturated fat and rich in whole grains, fruits, and vegetables.
- Properly treat long-term conditions, like high blood pressure, diabetes, and high cholesterol.
- Manage stress.
- Ask your doctor about taking a small, daily dose of aspirin.
- Although most people are able to tolerate such a low dose of aspirin, even this small amount can rarely lead to serious bleeding, particularly from the gastrointestinal (GI) tract.
- Aspirin may not work as well when combined with other pain medicines.