Definition
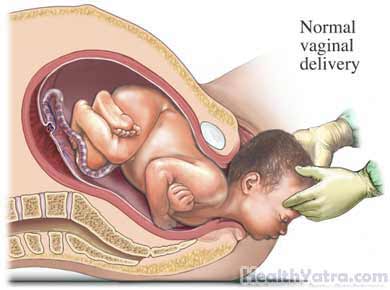
In a vaginal birth, the baby will come out through the birth canal. Most women give birth at around 38-41 weeks of pregnancy. However, there is no way to know exactly when you will go into labor.
Reasons for Procedure
Labor is the process that positions the baby for birth, delivers the baby out of the birth canal, and passes the placenta after birth.
Possible Complications
Your doctor will review a list of possible complications, which may include:
- Bleeding
- Uterine infection
- Tear of tissue around the vagina
- Complications requiring forceps, vacuum extraction, or cesarean delivery (C-section)
- Blood clots
- Injury to the baby
Some factors that may increase the risk of complications include:
- Anemia
- Diabetes
- Bleeding disorder
- Lung or heart disease
- Infectious disease (eg, active genital herpes infection, HIV)
- Water breaking before your contractions start
- Placenta previa (placenta positioned over the canal opening)
- Abruptio placenta (early separation of the placenta from the wall of the womb)
- Umbilical cord prolapse (umbilical cord slips out of the birth canal before the baby’s head)
- Large baby or a baby in the wrong position inside the womb
Be sure to discuss these risks with your doctor before giving birth.
What to Expect
Prior to Procedure
During pregnancy you should:
- Be sure to go to all prenatal care visits with your doctor
- Eat nutritiously and drink plenty of fluids.
- Get as much sleep as possible.
- Read about giving birth and take a childbirth class.
- Choose a support person to be with you during labor and delivery.
- Write a birth plan that explains what you want and helps you to think about possible complications.
- Talk to your doctor about:
- Ways to contact her after hours and when you should call
- Steps you should take when in labor
- Whether you want pain relief during labor
- Perineal massage—The perineum is the area between the anus and the vagina. Massaging it may help to reduce your chance of trauma to that area.
- How you will travel to the hospital
- Arrangements for home and work
- Be aware of the signs of labor, which include:
- Contractions
- “Water breaks” (amniotic fluid that surrounds the baby leaks out through the vagina)
- Back pain
- Slight vaginal bleeding
True Versus False Labor
Before “true” labor begins, you may have periods of “false” labor. These are irregular contractions of your uterus, called Braxton Hicks contractions. They are normal but can be painful. They are usually also felt in the stomach and not the back. Timing the contractions is a good way to tell the difference between true and false labor. Note how long it is from the start of one contraction to the start of the next. Keep a record for an hour. If the contractions are getting closer together, longer, stronger, and are being felt in your back, then it may be true labor. If you think you are in labor, call your doctor.
Birth Labor
During this process, you will prepare to deliver your baby. At the beginning of labor, the uterus (where the baby grows during pregnancy) will begin to contract, moving the baby down the vagina (birth canal). The cervix, the opening of the uterus into the vagina, will slowly enlarge to a diameter of about 10 centimeters. This will allow the baby to pass through and be delivered through the opening of the vagina. This process usually takes a while. However, if you have delivered vaginally before, labor can be very quick.
Anesthesia
Labor can cause severe pain, but keep in mind that every woman’s labor is different. Everyone experiences pain differently. While planning the delivery, talk to your doctor about your options for pain relief.
In the early stages of labor, techniques like rhythmic breathing, meditation, andacupressure may be helpful. Some women do not require any other pain control.
There are many medical options for pain control. All treatments to relieve pain during labor have risks and benefits. Make sure you discuss these with your doctor:
- Pain medicines by IV or muscle injection
- Given when contractions become stronger and more painful
- Can cross into the baby’s bloodstream
- Epidural block
- Liquid pain medicine injected near spinal cord
- Given in small amounts by an anesthesiologist (a doctor who specializes in anesthesia)
- Does not cross into baby’s bloodstream
- Decreases pain and feeling in your lower body
- Provides good pain relief and allows you to continue with delivery
- Can cause headaches and drop in blood pressure, as well as changes in baby’s heartbeat
- Spinal block
- Liquid pain medicine injected into spinal fluid
- Used for pain relief during delivery, especially if forceps or vacuum extraction is needed
- Often used for C-section
- Numbs lower half of the body and reduces your ability to push
- Provides good pain relief and works quickly
- Can cause headaches after delivery and drop in blood pressure during labor and delivery, as well as changes in baby’s heartbeat
- Local anesthesia
- Injected into vagina or surrounding area
- Used if an episiotomy (cutting near the vagina) is needed
- Also used when vaginal tears are stitched
- Does not relieve pain of contractions during labor
Description of the Procedure
Once the cervix is fully dilated (opened) and the baby seems to be heading down the birth canal, the nurses will help prepare you for delivery. Your legs may be draped with cloths. Some doctors will clean the area around the vagina with an antiseptic solution.
You may put your legs into holders, especially if you have an epidural. The nurses and your support people may hold your legs in a comfortable position. This will help you to push. Your doctor may encourage you to find a position that is right for you. Each time you have a contraction, you will be instructed to push. This involves you bearing down, like you are trying to have a bowel movement.
“Crowning” is when the baby’s head is seen at the opening to the vagina. When this happens, you may be asked to slow your pushing. Depending on your delivery plan, the doctor may massage your perineum to gently stretch it. An episiotomy is not routinely done, but in some cases, it is necessary.
Once your baby’s head is out, you will be asked to stop pushing. The doctor will check to make sure that the umbilical cord is not around the baby’s neck. Then, you will be able to push the rest of the baby out. If the baby appears healthy and is breathing well, he may be placed on your stomach. The umbilical cord will be clamped and cut. Within the next 20 minutes, the placenta will be delivered.
Sometimes the baby’s head does not move as expected through the birth canal. If this happens, your doctor may use forceps or vacuum extraction to move the baby.
Immediately After Procedure
- Right after birth, your baby may be placed on your abdomen or chest. This skin-to-skin contact may lead to improved breastfeeding success.
- You may need stitches if your perineum is cut or torn.
- You may receive abdominal massage to help the uterus clamp down and decrease bleeding.
- The vaginal area, perineum, and rectum will be cleansed.
- An ice pack will be placed on the perineum to soothe and decrease swelling.
- You may be given a shot of oxytocin to help decrease bleeding.
- The doctor will give you pain medicine.
How Long Will It Take?
The average time for you to deliver your first baby and the placenta is 12 hours. This can vary greatly, though.
Will It Hurt?
Labor causes severe pain during contractions. There may be brief periods of relief after each contraction. Talk to your doctor about your options for managing pain.
Average Hospital Stay
The usual length of stay for a vaginal delivery is 1-3 days. Your doctor may choose to keep you longer, however, if complications arise.
Post-procedure Care
Having a baby will change you physically and emotionally.
Physical Effects
Physically, you might have the following:
- Sore breasts—Your breasts may be painfully engorged when your milk comes in. Also, your nipples may be sore.
- Constipation—You may not be able to move your bowels until the third or fourth day after delivery.
- Stitches may make it painful to sit or walk.
- Hemorrhoids—Hemorrhoids are common. They may make it painful for you to move your bowels.
- Hot and cold flashes—This is due to your body trying to adjust to the change in hormones and blood flow levels.
- Urinary or fecal incontinence—During delivery, your muscles were stretched. This may make it hard for you to control your urine and bowel movements for a short period of time after delivery.
- “After pains”—The shrinking of your uterus can cause contractions. These can worsen when your baby nurses or when you take medicine to reduce bleeding. It is normal to have this after delivery.
- Vaginal discharge—This is heavier than your period and often contains clots. The discharge gradually fades to white or yellow and stops within two months.
- Weight—Your postpartum weight will probably be about 10 pounds below your full-term weight. Water weight drops off within the first week as your body regains its salt balance.
Emotional Effects
Emotionally, you may be feeling:
- “Baby blues”—About 80% of new moms have irritability, sadness, crying, oranxiety. This begins within days or weeks of giving birth. These feelings can result from hormonal changes, exhaustion, unexpected birth experiences, adjustments to changing roles, and a sense of lack of control over your new life.
- Postpartum depression (PPD)—This condition is more serious and happens in 10%-20% of new moms. It may cause mood swings, anxiety, guilt, and persistent sadness. Your baby may be several months old before PPD strikes. It is more common in women with a family history of depression.
- Postpartum psychosis—Postpartum psychosis is a rare, but severe condition. Symptoms include difficulty thinking and thoughts of harming the baby. If you feel this way, call your doctor right away.
- Sexual relations—You may not feel physically or emotionally ready to begin sexual relations right away. In most cases, you will feel more interested in sex in a few weeks.
Ways to Take Care of Yourself
- When your baby sleeps, take a nap.
- Set aside time each day to relax with a book, or listen to music.
- Ask your doctor about when it is safe to shower, bathe, or soak in water.
- Get plenty of exercise and fresh air.
- Schedule regular time for you and your partner to be alone and talk.
- Make time each day to enjoy your baby. Encourage your partner to do so, too.
- Breastfeeding is encouraged unless your doctor tells you otherwise
- Clean less and have easier meals. Take a break from having visitors if you feel stressed.
- Ask for help when you need it.
- Talk with other new moms and create your own support group.
- Delay having sexual intercourse and putting any objects into the vagina until you have had your 4-6 week check-up
- Be sure to follow your doctor’s instructions.
Call Your Doctor
After you leave the hospital, contact your doctor if any of the following occur:
- Signs of infection, including fever and chills
- Increased bleeding: soaking more than one sanitary pad an hour
- Wounds that become red, swollen, or drain pus
- Vaginal discharge that smells foul
- New pain, swelling, or tenderness in your legs
- Pain that you cannot control with the medicines you have been given
- Pain, burning, urgency or frequency of urination, or persistent blood in the urine
- Cough, shortness of breath, or chest pain
- Depression, suicidal thoughts, or feelings of harming your baby
- Breasts that are hot, red, and accompanied by fever
- Any cracking or bleeding from the nipple or areola (the dark-colored area of the breast)
In case of an emergency, call for medical help right away.
